International Medical Assistance · Since 2000
Trusted by Leading Insurers & Partners




















The people we take care of
A diplomat's child with a fever in Bogotá. An executive who needs surgery in Miami. A student who broke her ankle in Barcelona. These aren't files — they're people who need someone to coordinate their care, manage their costs, and get them home safely. That's what we do, and we've been doing it for 26 years.
Embassy & Diplomatic Families
Consular staff, ambassadors, and their dependents posted abroad who need reliable medical access in unfamiliar healthcare systems.
Multinational Corporate Families
Executives, relocating employees, and their families covered by international group health or travel policies through their employer.
Global Nomads & Remote Workers
Digital nomads, long-term travelers, and remote workers living across borders who need consistent healthcare coordination.
International Students
Exchange students, university attendees, and study-abroad participants covered by school-required or parent-purchased insurance.
Retirees & Snowbirds
Expat retirees and seasonal travelers who spend extended periods abroad and need coordination between home-country insurers and local providers.
Leisure & Adventure Travelers
Vacationers, cruise passengers, and adventure tourists with travel assistance or trip insurance who encounter medical emergencies abroad.
What makes us different
One partner, not five vendors
Clinical coordination, cost containment, claims financing, provider payments, and technology — all under one roof. You don't need to stitch together separate companies. We built the whole stack.
The deepest network in the Americas
500+ directly contracted hospitals across 6 continents. 300+ in Latin America alone. Aetna PPO access in all 50 U.S. states. From Mayo Clinic to Albert Einstein São Paulo — we don’t just have contracts, we have relationships.
We pay providers fast — and you save money
We finance claims from our own balance sheet. Providers get paid in days instead of months. In return, they give us meaningful discounts — and we pass those savings directly to you.
U.S. claims cost 37–52% less
The U.S. is where international claims get painful. Smart triage diverts 50% of calls from the ER. Aetna PPO rates cut hospital charges by 52% on average. Hospitalists reduce length of stay. AI adjudication catches overbilling. The result: your U.S. claims cost dramatically less.
Technology that replaces paperwork
MDiX handles claims adjudication in minutes, not weeks. Virtual debit cards replace wire transfers. Provider portals replace fax machines. We automate the tedious so your team can focus on what matters.
Always on. Three cities. Five languages.
Our teams in Miami, São Paulo, and Buenos Aires cover every time zone in the Americas. English, Spanish, Portuguese, German, Italian — around the clock, every day of the year. Twenty-six years and counting without going offline.
What it looks like to work with us
Typical Fragmented Model
MDabroad Fulfillment Model ✓
“Switching to MDabroad reduced our U.S. inpatient claims cost by 41% in the first year. The combination of Aetna PPO access, hospitalist deployment, and claims financing is something no other vendor offered us as a single package.”
Everything your members need. One platform.
Assistance & Cost Containment
Members get help in under 60 seconds. Nurse triage, physician deployment, medical evacuations, and U.S. cost interventions that reduce claims 37–52%.
Learn more →Claims Financing
Providers get paid in days, not months. Insurers benefit from significant savings — up to 37% on U.S. claims — without deploying a dollar of capital.
Learn more →MDiX Platform
Claims adjudicated in minutes, not weeks. Virtual debit cards replace wire transfers. Provider portals replace fax machines. One API for everything.
Learn more →Telemedicine
A doctor in your language in under 5 minutes. 50% of calls resolve without an ER visit — better outcomes, lower loss ratios.
Learn more →Pharmacy & PBM
Direct billing in the U.S. through PBM networks. Members pay $0 at the counter. Specialty pharmacy navigator for biologics and high-cost therapies.
Learn more →Parametric & Virtual Card
Flight delayed? Paid automatically. No claim form, no phone call. Virtual debit cards for instant member payouts at point of care.
Learn more →Reliability & Operations
26 years, zero days offline. Three cities, five languages, around the clock. Built to handle COVID surges, hurricane seasons, and holiday peaks.
Learn more →Assistance & Cost Containment
When someone calls at 3am, we answer.
Our alarm center never closes. A nurse picks up, triages in the caller's language, and coordinates everything — from a telemedicine consult that saves an ER visit, to a medical evacuation that saves a life. We deploy hospitalists to manage inpatient care in real time. We negotiate directly with providers. We handle the paperwork so your member can focus on getting better.
- Nurse-led triage and multilingual physician consultations in English, Spanish, and Portuguese
- U.S. hospitalist deployment and inpatient case management in real time
- UCR benchmarking, direct negotiation, and fraud prevention on every claim
- Medical evacuations, repatriation, house calls, and consular support
U.S. hospital costs are the #1 problem. We built the solution.
For international insurers, U.S. hospital bills are where claims get painful. A single inpatient stay can run into six figures. Our approach combines network discounts, clinical intervention, and smart technology to bring those numbers down — materially and consistently. Here's how.
Smart Triage
Every traveler's first contact is a telemedicine physician — ensuring appropriate care immediately. Great for members, great for loss ratios.
Aetna PPO Network Access
Direct access to the Aetna network delivers an average 52% discount on U.S. hospital charges with best-in-class facilities.
Hospitalist Deployment
Place hospitalists to manage inpatient decisions, reduce length of stay, and guide clinical choices in real time.
UCR + AI Adjudication
Adjudicate against UCR benchmarks with AI-powered pricing checks, fraud detection, and real-time validation.
Claims Financing
MDabroad finances claims promptly, capturing provider discounts that translate into lower net costs for the insurer — subject to agreed payment terms.
52% Avg. U.S. Discount
Aetna PPO network access across all 50 states. A $200K inpatient stay becomes $96K before any further negotiation.
50% Fewer ER Visits
First-contact telemedicine resolves half of all cases without an emergency room visit — saving $8K–$25K per diverted case.
3–5 Day Settlement
AI-powered adjudication and balance-sheet financing close claims in days, not the 60–90 day industry standard.
Claims Financing for Insurers
We pay providers fast. You save on every claim.
Here's how it works: when a hospital knows they'll get paid in days instead of months, they'll agree to a lower price. We put up the capital. We manage the collection. And the discount — up to 37% on U.S. claims — translates directly into lower net costs for you. Providers are happier, your claims cost less, and the entire process runs on agreed payment schedules between you and MDabroad.
- MDabroad finances claims upfront — insurers deploy zero capital
- Prompt payment unlocks provider discounts of up to 37% on U.S. claims
- Significant discount savings reduce your net claims cost — subject to agreed payment terms
- Integrated OCR + AI adjudication validates every claim before funding
- Replenishable technical accounts with transparent monthly reconciliation
- Full audit trail, capped exposure limits, and role-based funding approvals
How It Works: From Claim to Insurer Savings
Admission & VOB
Verify benefits and issue letter of guarantee to the provider.
Invoice & Validation
Provider submits via MDiX. OCR + AI adjudicates and detects fraud.
MDabroad Finances
We pay the provider promptly from our balance sheet, securing a discount.
Discount Passed to Insurer
The insurer receives a reduced claim amount — the discount is yours.
Reconciliation
Monthly reconciliation via replenishable technical accounts with full audit trail.
Insurer Reconciliation
Documentation and collections management.
Flexible Commercial Models
Every insurer’s claims portfolio is different. We offer three financing structures — each designed to align incentives between insurer, provider, and MDabroad.
Immediate Settlement
We pay the provider upfront from our balance sheet. You reimburse us on agreed terms. Providers get paid fast, you get a discount. Simple.
Shared Savings
We negotiate the discount, advance the net, and share the captured value with you. The more we save, the more you save. Aligned incentives.
Capitated Facility
A pre-funded monthly facility with dynamic limits for high-volume partnerships. Predictable cash flow, maximum discount capture. Built for scale.
6,000+ U.S. hospitals. 500+ direct partners. White-glove concierge service.
High-touch, concierge-level coordination is what sets MDabroad apart. We don't just connect calls — we deploy hospitalists, negotiate GOP acceptance in real time, and manage every case end-to-end. In the U.S., our Aetna PPO access covers 6,093 hospitals across all 50 states. In Latin America, we know the billing teams, international patient coordinators, and physicians by name. When a case lands at 2am, that relationship is the difference between a smooth admission and a bureaucratic nightmare.




































“We typically wait over 60 days to get paid from insurers. MDabroad gives us an opportunity to get paid within just days of sending invoices. We actually look forward to receiving their GOP.”
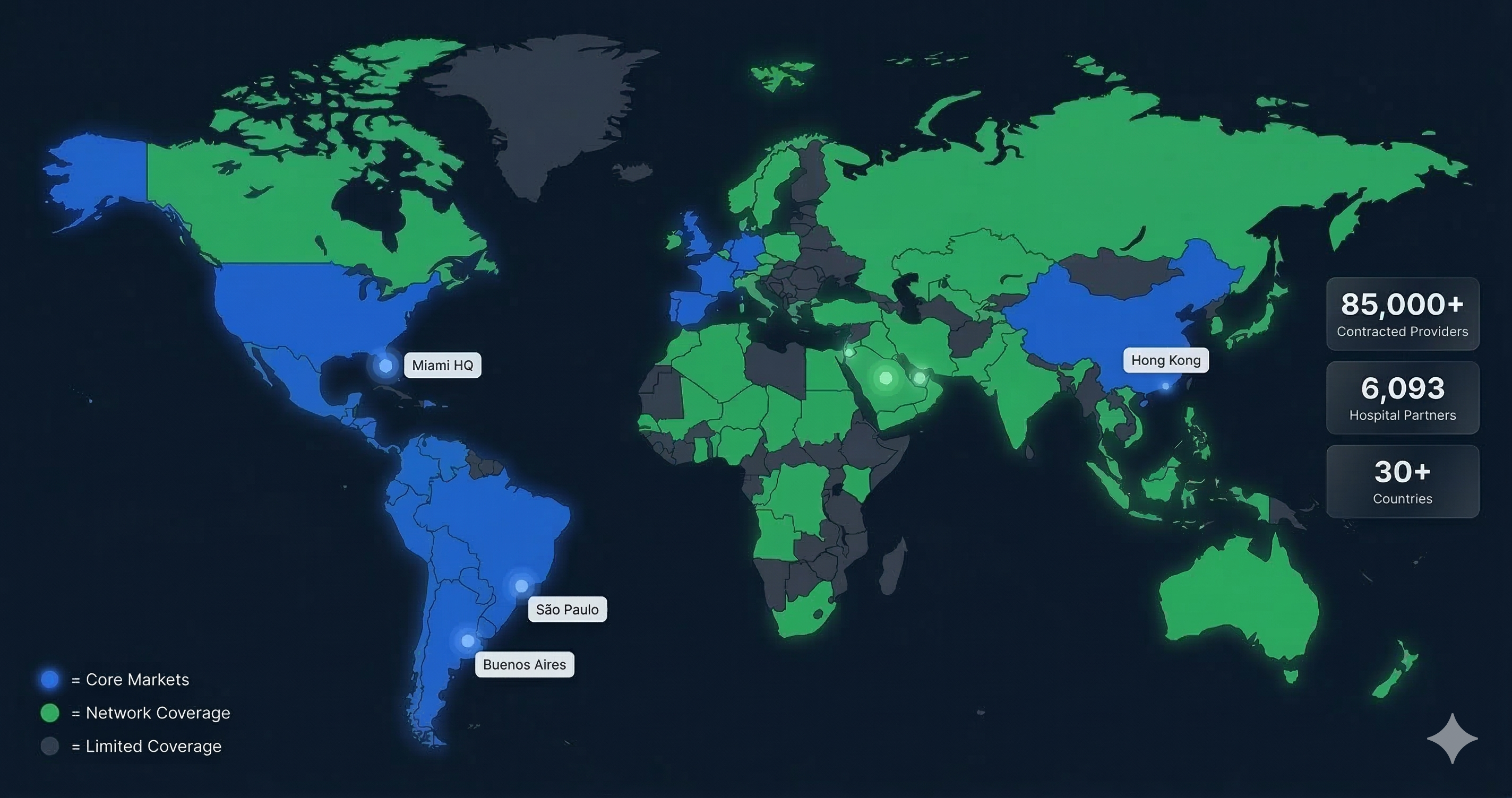
Become an MDabroad Network Provider
Join hundreds of hospitals and medical centers worldwide that benefit from MDabroad's claims infrastructure. Network providers receive immediate settlement, reduced administrative burden, and access to a growing flow of international patients.
- Immediate payment via claims financing — no waiting 90+ days
- Direct benefit verification and letter of guarantee via MDiX
- Dedicated case manager for every international patient
- Multi-currency settlement in your local currency
- Real-time claim status tracking and transparent pricing
- Access to growing volume of insured international travelers
Assistance Partners Worldwide
In the 150+ countries where we don’t operate directly, our vetted partner network ensures seamless local coordination — from Bangkok to Berlin, every region covered by a provider who knows that market. When a member calls from Singapore, our partner in Asia handles the ground coordination while our team manages the case end-to-end.
























Claims adjudicated in minutes. Not weeks.
Most claims sit in a queue for days. Ours go through AI-powered validation the moment they arrive — OCR extracts invoice data, checks against UCR benchmarks, flags anomalies, applies negotiated discounts, and produces an audit-ready decision. The entire cycle takes minutes.
Virtual Debit Card
No wire transfers. No waiting. Just a card that works.
Issue a virtual debit card to your member or directly to a provider — instantly. Members can pay out-of-pocket expenses on the spot. Providers get guaranteed payment without chasing paperwork. It's the fastest way to move money in international healthcare.
- Instant issuance — virtual card delivered in seconds via MDiX
- Members pay providers directly, eliminating reimbursement delays
- Providers receive guaranteed payment at point of care
- Full integration with claims workflow — every transaction tracked
Parametric Insurance
Flight delayed? Luggage lost? Paid automatically.
Integrated with Blink Parametric, MDabroad offers travel disruption products that trigger automatically — no claim form, no phone call, no waiting. When a flight delay is detected or luggage goes missing, payout happens on its own. Your members experience insurance the way it should work.
- Flight delay: auto-triggers when delay is detected — no manual claim
- Lost luggage: parametric payout within hours, not days
- Single API via MDiX — add parametric alongside medical assistance
- A genuinely modern traveler experience that differentiates your product
MDiX: The technology that makes all of this work.
Instant Claims Adjudication
AI-powered engine processes claims in minutes, not weeks. OCR extracts invoice data, validates charges against UCR benchmarks, detects fraud patterns, and applies negotiated discounts — all automatically with full audit trail.
Virtual Debit Card Payments
Issue virtual debit cards instantly for member reimbursements and upfront provider payments. Eliminates out-of-pocket burden for travelers and removes wire-transfer delays for facilities. Fully integrated with claims workflow.
Parametric Payouts
Integrated with Blink Parametric for auto-triggered payouts on flight delays and lost luggage — no manual claims process required. Event detection triggers instant settlement via virtual card or bank transfer.
Provider Portal
Hospitals and clinics submit invoices digitally, track claim status in real time, view payment history, manage Letters of Guarantee, and communicate with case managers — all through a single secure interface.
Implementation Roadmap
Phase 1: Core Infrastructure
Instant claims adjudication, virtual debit card payments, provider portal, real-time VOB, security hardening, and audit logging.
Phase 2: Intelligence & Automation
Agentic bots, predictive analytics, member self-service portal, parametric payout engine, and automated provider onboarding.
Phase 3: Ecosystem & Scale
White-label portal suite, insurer BI dashboards, third-party API marketplace, parametric product builder, and multi-tenant architecture.
Developer Event Model
claim.submitted → OCR + AI adjudication triggered
claim.adjudicated → Discount applied, fraud check passed
claim.payment.initiated → Virtual debit card issued or wire sent
provider.payment.settled → Multi-currency settlement confirmed
parametric.event.detected → Auto-payout triggered (flight delay, luggage)
portal.invoice.uploaded → Provider claim enters adjudication queue
member.reimbursement.issued → Virtual card loaded or bank transfer sentRESTful endpoints with OAuth 2.0 or API keys. Webhook reliability with retries, idempotency keys, and status callbacks.
Telemedicine
A doctor in your language, in minutes.
Before anyone goes to an emergency room, they talk to us. A nurse screens the call. A physician consults — in the member’s language. Half of all cases resolve right there. No ambulance. No ER copay. No $12,000 surprise bill. Just a diagnosis, a prescription, and peace of mind.
That single triage step diverts thousands of sub-acute cases every year — cutting ER utilization in half and saving insurers between $8,000 and $25,000 per diverted case.
- Physician video consult in under 5 minutes — EN, ES, PT, DE, FR — with real-time AI translation for 20+ additional languages
- 50% of cases resolved without an ER visit — better member experience, dramatically lower loss ratios
- E-prescribing with pharmacy delivery coordination — medication at the member’s hotel or home
- Mobile app with SOS alerts, on-demand telehealth, and digital ID card for instant provider verification
Pharmacy Benefits
U.S. drug prices are 278% higher. You need a partner who knows this.
According to RAND, Americans pay 2.78× more for prescription drugs than the rest of the developed world. For brand-name medications, it’s 3.22×. A single biologic can run $185,000 a year in the U.S. — and your member just got diagnosed abroad. MDabroad eliminates the sticker shock. We bill insurers directly through Aetna/CVS Caremark and partner PBM networks, so members pay nothing at the counter. For specialty medications, our pharmacy navigator sources each drug at the best available price and manages the entire fulfillment process.
- Direct PBM billing — members pay $0 at the counter; we settle with the insurer through major U.S. PBM networks
- Specialty Rx navigation — 340B access, manufacturer programs, and competitive sourcing for biologics, chemo, and targeted therapies
- One navigator per case — a single point of contact who handles prior auth, pricing, and fulfillment end-to-end
Reliability & Operations
Twenty-six years. Zero days offline.
COVID surges, hurricane seasons, geopolitical crises, holiday travel peaks — our operations center in Buenos Aires has handled all of it without a single day of downtime. When your members need help, the system has to work. Ours does.
- Five-language operations (EN/ES/PT/DE/IT) with real-time AI translation for additional languages on demand
- Zero-downtime track record through COVID, hurricanes, and geopolitical disruptions — elastic staffing handles any surge
- Agentic automation handles document collection, scheduling, follow-ups, and status updates autonomously
- ISO 27001 hardened infrastructure with WAF, SIEM, edge caching, and automated failover
“My daughter was hospitalized in Buenos Aires at 2am. MDabroad had a case manager at the hospital within the hour, coordinated the entire stay, negotiated with the provider, and arranged the transfer home. I’ve never experienced anything like it.”
Built in the Americas. Serving the world.
MDabroad started in 2000 with a simple observation: when someone gets sick far from home, the system fails them. Providers don't get paid. Insurers can't see what's happening. And the person in the hospital bed is left waiting. We built the infrastructure to fix that — clinical coordination, cost containment, claims financing, and a technology platform that ties it all together. Twenty-six years later, we've managed over a billion dollars in medical claims across 150+ countries, from our offices in Miami, São Paulo, and Buenos Aires.
Our Mission
Take care of people far from home — and make the economics work for everyone involved. Lower costs for insurers. Faster payments for providers. Better outcomes for the person who matters most.
Our Vision
A world where getting sick abroad doesn't mean getting lost in the system. Where claims are settled in minutes, not months. Where the infrastructure just works — quietly, reliably, across borders.
Our Values
- Clinical integrity & patient-first care
- Independence & transparency
- Platform reliability & continuous improvement
- Commercial discipline — measurable ROI
- Operational excellence through resilient execution
São Paulo, Brasil
Av. Paulista, 1842 — Torre Norte, Conj. 155
Bela Vista, São Paulo, SP
CEP 01310-945
Buenos Aires, Argentina
Esmeralda 1080, Piso 7, Dpto. A
Ciudad de Buenos Aires (C1007ABR)
Our Team
Enterprise-Grade Trust & Compliance
MDabroad handles Protected Health Information under HIPAA and GDPR standards and maintains technical and administrative safeguards.
Access Control
Role-based access control with audit logging on all system actions.
Encryption
All data encrypted in transit (TLS) and at rest. PHI follows minimum necessary disclosure.
Monitoring & Response
SIEM integration, continuous monitoring, periodic penetration testing.
Configuration & Compliance
Configuration management, malware detection, and ISO-aligned hardening.
Cross-border transfers are subject to contractual safeguards and minimal necessary disclosure. MDabroad maintains full compliance with applicable data protection regulations.
Tailored Solutions for Every Stakeholder
For Insurers & TPAs
Reduce cost-per-claim, accelerate settlements, improve loss ratios. Claims financing, U.S. cost containment, and MDiX automation.
Request Insurer Demo →For Providers & Hospitals
Improve cash flow, reduce administrative burden, grow international patient business.
Provider Onboarding →For Members & Travelers
24/7/365 multilingual support, telemedicine, pharmacy delivery, emergency coordination.
Start a Claim →For Partners & Distributors
White-label assistance and claims infrastructure. Branded solutions, API access, embedded capabilities.
Partner With Us →Ready to Evaluate MDabroad? Start Here.
Whether you're an insurer, TPA, reinsurer, or self-insured employer issuing a request for proposal, MDabroad makes it easy. Download our capabilities deck, review our standard RFP responses, or submit your RFP directly and our commercial team will respond within 48 hours.
Capabilities Deck
Download our comprehensive overview: services, technology, network, compliance, and commercial models.
Download PDF →Pre-Built RFP Responses
Access standard answers to common RFP questions covering SLAs, clinical protocols, technology, data security, and pricing.
View Responses →Submit Your RFP
Send us your RFP document and requirements. Our commercial team will deliver a tailored response within 48 business hours.
Submit an RFP
From the MDabroad Team
Follow MDabroad and our leadership team on LinkedIn for the latest insights on international medical claims and industry developments.
The U.S. remains the most expensive destination for international medical claims. Our hospitalist-first model is delivering measurable cost reductions on high-acuity cases.
MDiX Phase 2 is live: agentic bots now handle case follow-ups, document collection, and appointment scheduling autonomously.
Excited to announce new provider partnerships across Southeast Asia. Our global hospital network now spans 6 continents with direct billing.
From our team
Introducing the MDabroad Insights Feed
Industry intelligence, market analysis, and operational insights from 26 years at the intersection of international health insurance and medical assistance.
Why U.S. Hospital Claims Cost 37–52% Less with MDabroad
Direct provider contracts, AI-powered repricing, hospitalist deployment, and local-currency settlement eliminate the markup layers that inflate international medical claims.
How Balance-Sheet Financing Unlocks Provider Discounts
Guaranteed 72-hour payment terms give MDabroad negotiating leverage that translates into deeper discounts passed directly to payer clients.
Contact MDabroad
Have a question, want to discuss partnership opportunities, or need assistance? Fill out the form below and our team will respond within one business day.
Frequently Asked Questions
Everything insurers, providers, and partners need to know about MDabroad’s international medical assistance, claims financing, and technology platform.
About MDabroad
Assistance & Clinical Coordination
Claims Financing
MDiX Technology Platform
Provider Network
Security & Compliance
Parametric & Virtual Card
Getting Started
“When a major assistance event occurs, the difference between a 40% and 70% loss ratio often comes down to one factor: who is managing the case on the ground.”
Need a partner for cost and fulfillment?
We can put together a complete response covering network access, compliance posture, white-label operations, and implementation timelines. Your procurement team gets what they need. You get a partner who actually delivers.







